This podcast episode is worth 0.34 CPD credits. Upgrade to Pro
In this episode, Dr Roger Henderson explores an important and often overlooked area of head and neck oncology: oral mucosal cancer. As GPs, we frequently encounter oral lesions in primary care, and they are also often seen in dental practice, emergency settings and specialist clinics; however, distinguishing benign conditions from early malignancy can be challenging. Here, we break down the essential anatomy of the oral cavity, clarify how it differs from the oropharynx and examine the major risk factors driving disease development, including tobacco, alcohol, human papillomavirus (HPV) and immunosuppression. We also discuss clinical presentation, red-flag features, diagnostic pathways, staging principles and current management strategies. Most importantly, we focus on the role GPs play in early detection, timely referral and multidisciplinary care.
Key take-home points
- Oral mucosal cancer arises from the epithelial lining of the oral cavity, including the lips, buccal mucosa, anterior two-thirds of the tongue, floor of the mouth, hard palate, gingiva and retromolar trigone.
- Clear anatomical distinction between the oral cavity and oropharynx is essential because tumour behaviour, staging and treatment strategies differ significantly between these regions.
- Squamous cell carcinoma accounts for more than 90% of oral cavity malignancies.
- Tobacco use is the single most significant risk factor for oral mucosal cancer. The risk increases substantially when combined with alcohol consumption, due to a synergistic carcinogenic effect.
- Smokeless tobacco products, including chewing tobacco, snuff and betel quid, significantly increase the risk of oral cavity cancers, due to prolonged mucosal exposure to carcinogens.
- Alcohol enhances mucosal permeability, facilitating the penetration of carcinogens into epithelial tissues and increasing malignant potential.
- HPV, particularly types 16 and 18, is strongly associated with oropharyngeal cancers. Its role in oral cavity cancers is less clearly defined but remains under investigation.
- Patients who have undergone haematopoietic stem cell or solid organ transplantation are at increased risk of oral malignancies. Chronic immunosuppression and graft-versus-host disease contribute to malignant transformation.
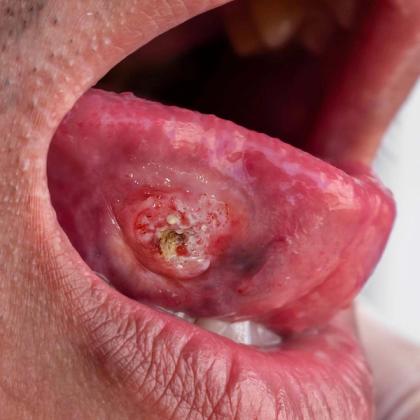
- Early-stage oral mucosal cancer may present as persistent white, red or mixed mucosal patches that do not resolve.
- Advanced disease may manifest with induration, ulceration, dysphagia, odynophagia, weight loss and cervical lymphadenopathy.
- Biopsy is essential for definitive diagnosis of any suspicious oral lesion persisting beyond 2 weeks. Imaging and endoscopic evaluation are critical for accurate staging and detection of synchronous tumours.
- Depth of invasion is a key factor in TNM staging (tumour size/extent, lymph node involvement and metastasis) and has significant prognostic implications.
- Surgery is the primary treatment modality for most oral cavity cancers, particularly in early-stage disease. Advanced cases often require multimodality therapy including radiotherapy, chemotherapy or immunotherapy.
- Lymph node involvement and extranodal extension are associated with significantly poorer prognosis.
- Early detection and timely intervention dramatically improve survival outcomes, with 5-year survival rates significantly higher in localised disease compared to regional or distant spread.
Key references
- Renou A, et al. J Clin Med. 2023;12(3):1071. doi: 10.3390/jcm12031071.
- Rivera C. Int J Clin Exp Pathol. 2015;8(9):11884-11894.
- Rochefort J, et al. Front Oncol. 2023;12:1068979. doi: 10.3389/fonc.2022.1068979.
- NICE. 2018. https://www.nice.org.uk/guidance/ng36.
- Wang B, et al. Chin J Cancer. 2013;32(11):614-618. doi: 10.5732/cjc.012.10219.
- Kato G, et al. World J Otorhinolaryngol Head Neck Surg. 2020;6(1):66-75. doi: 10.1016/j.wjorl.2019.06.001.
Create an account to add page annotations
Annotations allow you to add information to this page that would be handy to have on hand during a consultation. E.g. a website or number. This information will always show when you visit this page.