This podcast episode is worth 0.26 CPD credits. Upgrade to Pro
Basal cell carcinoma (BCC) is a diagnosis most GPs encounter regularly, yet its familiarity often disguises its true impact. As the most common cancer in humans, BCC shapes clinical workload, healthcare costs and patient quality of life far more than its low mortality rate suggests. Although it is frequently described as slow growing and low risk, delayed recognition or inadequate treatment can lead to significant local destruction, functional impairment and disfigurement. In this episode, Dr Roger Henderson takes a closer look at BCC beyond the surface, exploring its clinical variability, underlying biology and evolving management strategies.
Key take-home points
- BCC is the most common cancer in humans and its rising incidence reflects both increased ultraviolet (UV) exposure and improved detection.
- Although metastasis is rare, BCC can cause significant local tissue destruction, particularly when diagnosis or treatment is delayed.
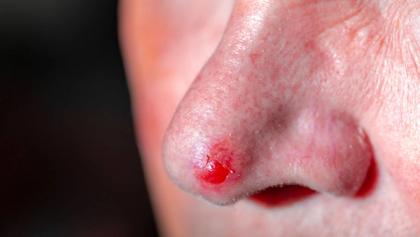
- The classic pearly papule with telangiectasia represents only a fraction of BCC presentations. Many lesions are subtle, atypical and easily misdiagnosed as benign or inflammatory conditions.
- Early-life UV exposure, especially intermittent and intense sun exposure during childhood, plays a critical role in future BCC risk.
- A notable proportion of BCCs arise on non–sun-exposed skin, highlighting the importance of additional risk factors beyond UV radiation.
- Dysregulation of the Hedgehog signalling pathway is central to BCC pathogenesis and has directly informed modern systemic therapies.
- Histologic subtype strongly influences tumour behaviour and treatment decisions. Infiltrative, morpheaform and micronodular variants carry higher recurrence rates and often extend beyond clinically visible margins.
- Biopsy confirms the diagnosis but may underestimate aggressive features, making clinicopathologic correlation essential.
- Mohs micrographic surgery offers the highest cure rates and is particularly valuable for high-risk, recurrent or anatomically sensitive tumours.
- Conservative treatments such as curettage, cryotherapy or topical therapy are effective only when carefully matched to low-risk disease.
- Radiation therapy is an important alternative when surgery is contraindicated; however, long-term cosmetic changes and the risk of secondary malignancies must be considered, especially in younger patients.
- Systemic Hedgehog pathway inhibitors have expanded options for advanced or unresectable BCC but are frequently limited by adverse effects.
- Immunotherapy is emerging as a treatment option for patients who fail or cannot tolerate Hedgehog pathway inhibition.
- A prior diagnosis of BCC significantly increases the risk of future tumours, necessitating long-term or lifelong dermatologic surveillance.
- BCC is rarely fatal, but its cumulative morbidity is substantial. Repeated treatments, cosmetic impact and functional impairment contribute to a significant quality-of-life and healthcare burden.
Key references
- Dika E, et al. Int J Mol Sci. 2020;21(15):5572. doi: 10.3390/ijms21155572.
- NICE. 2026. https://www.nice.org.uk/guidance/NG12/.
- Fania L, et al. Biomedicines. 2020;8(11):449. doi: 10.3390/biomedicines8110449.
- Thomson J, et al. Cochrane Database Syst Rev. 2020;11(11):CD003412. doi: 10.1002/14651858.CD003412.pub3.
Create an account to add page annotations
Annotations allow you to add information to this page that would be handy to have on hand during a consultation. E.g. a website or number. This information will always show when you visit this page.