Ovarian cancer
Ovarian cancer is the 5th most common malignancy in females in the UK accounting for 4275 deaths per year. Five thousand new cases are diagnosed each year - an incidence of 20.3 per 100 000 of the population.
Ovarian carcinoma accounts for a quarter of all genital tract cancer but is responsible for more than half the deaths, primarily due to its late presentation.
Most are adenocarcinomas - serous, mucoid and endometrioid; dysgerminoma, granulosa cell and metastatic tumours account for most of the remainder.
Ovarian carcinoma has a lifetime incidence of about 0.97%. This compares with carcinoma of the cervix, endometrium and breast which have lifetime incidences of 1.29%, 1.02% and 5.11% respectively. Ovarian carcinoma has a mean age of incidence of 58 years and usually occurs between the 3rd and 8th decades.
- the outcome for women with ovarian cancer is generally poor, with an overall 5 year survival rate of less than 35% (2)
- despite the relatively poor overall survival rates for ovarian cancer, there has been a two-fold increase in survival over the last 30 years. This has coincided with the advent of effective chemotherapy, and the introduction of platinum-based agents in particular, as well as changes in surgical practice (1)
Risk factors include older age, family history of breast or ovarian cancer, endometriosis, and nulliparity (3)
- hereditary factors are associated with 25% of cases, predominantly linked to BRCA1/2 gene variants
NICE guidance has emphasised the importance of clinicians being aware of the symptoms and signs of possible ovarian cancer (1):
- awareness of symptoms and signs
- refer the woman urgently if physical examination identifies ascites and/or a pelvic or abdominal mass (which is not obviously uterine fibroids
- carry out tests in primary care (see below) if a woman (especially if 50 or over) reports having any of the following symptoms on a persistent or frequent basis - particularly more than 12 times per month:
- persistent abdominal distension (women often refer to this as 'bloating')
- feeling full (early satiety) and/or loss of appetite
- pelvic or abdominal pain
- increased urinary urgency and/or frequency
- consider carrying out tests in primary care (see below) if a woman reports unexplained weight loss, fatigue or changes in bowel habit
- advise any woman who is not suspected of having ovarian cancer to return to her GP if her symptoms become more frequent and/or persistent
- carry out appropriate tests for ovarian cancer (see below) in any woman of 50 or over who has experienced symptoms within the last 12 months that suggest irritable bowel syndrome (IBS) , because IBS rarely presents for the first time in women of this age
- refer the woman urgently if physical examination identifies ascites and/or a pelvic or abdominal mass (which is not obviously uterine fibroids
- primary care testing for possible ovarian cancer
- measure serum CA125 in primary care in women with symptoms that suggest ovarian cancer
- if serum CA125 is 35 IU/ml or greater, arrange an ultrasound scan of the abdomen and pelvis
- f the ultrasound suggests ovarian cancer, refer the woman urgently for further investigation
- for any woman who has normal serum CA125 (less than 35 IU/ml), or CA125 of 35 IU/ml or greater but a normal ultrasound:
- assess her carefully for other clinical causes of her symptoms and investigate if appropriate
- if no other clinical cause is apparent, advise her to return to her GP if her symptoms become more frequent and/or persistent
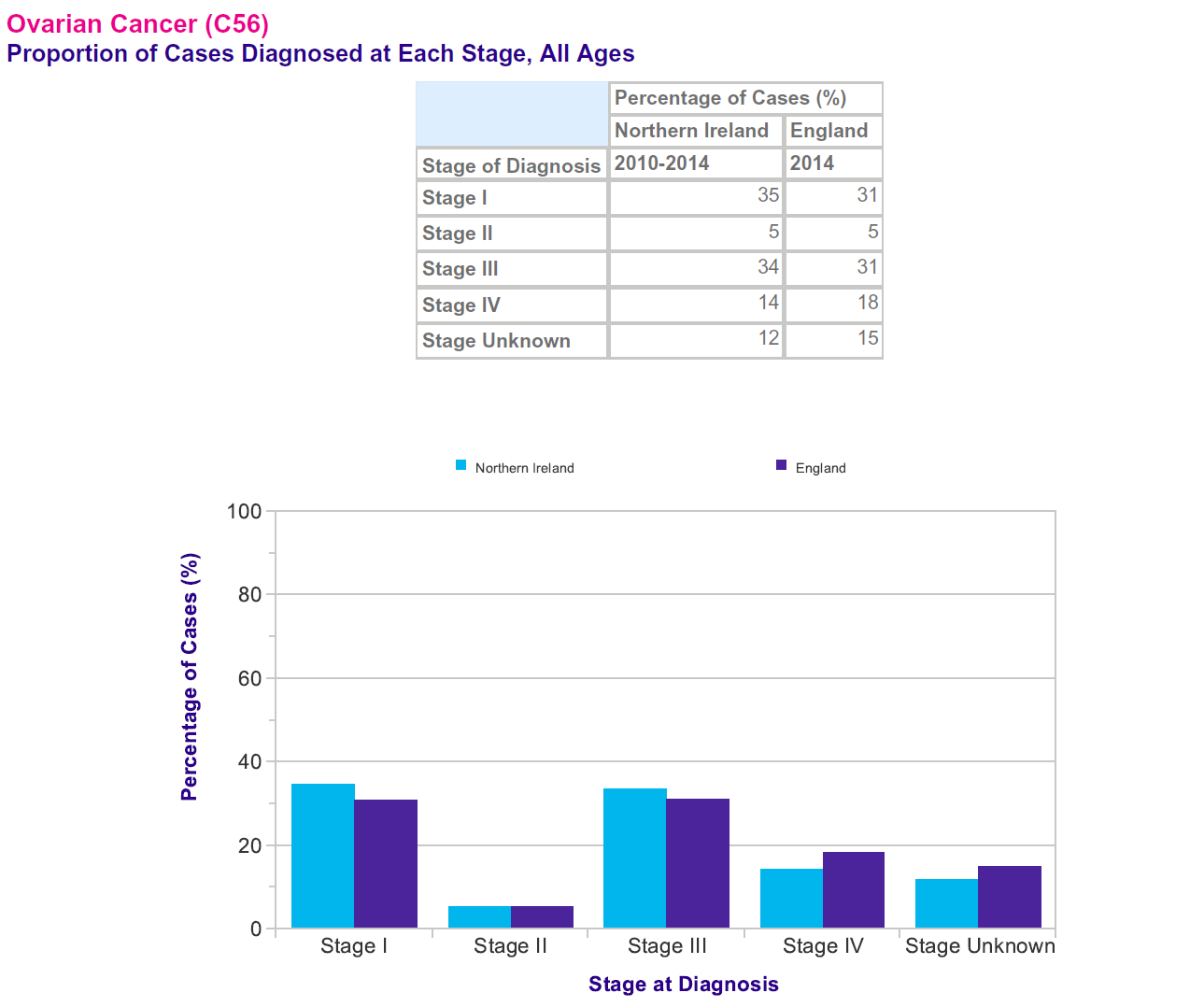
More females with a known stage are diagnosed at a late stage (55-58% are diagnosed at stage III or IV), than an early stage (42-45% are diagnosed at stage I or II). Between 17% and 21% of females have metastases at diagnosis (stage IV) (2)
Management principles (3):
- first-line treatment of early-stage ovarian cancer is surgery and adjuvant platinum-based chemotherapy
- for early-stage ovarian cancer, defined as limited to the ovary or fallopian tube (stage I) or confined to the pelvis (stage II), treatment is surgery (hysterectomy, bilateral salpingo-oophorectomy, omentectomy, and lymphadenectomy), followed by adjuvant chemotherapy (carboplatin and paclitaxel)
- treatment of advanced-stage ovarian cancer includes cytoreductive surgery, platinum-based chemotherapy, and targeted maintenance therapies such as bevacizumab and/or poly–adenosine diphosphate ribose polymerase (PARP) inhibitors
Patient information:
Useful information describing symptoms and signs of ovarian cancer is available on the website http://www.ovarian.org.uk/
References:
- NICE. Ovarian cancer: recognition and initial management. Clinical guideline CG122. Published: 27 April 2011 Last updated: 02 October 2023
- Ovarian cancer statistics. Cancer Research UK. Online 2024.
- Caruso G, Weroha SJ, Cliby W. Ovarian Cancer: A Review. JAMA. 2025;334(14):1278–1291.
Related pages
- Classification
- Epidemiology
- Risk factors
- Clinical features
- Screening (for ovarian cancer)
- Diagnosis and investigation
- Spread
- Staging of ovarian cancer
- Management
- Prognosis of ovarian cancer
- Gynaecological cancer (NICE urgent referral guidance for suspected cancer)
- Female genital tract cancers
- Referral criteria for ovarian cancer - genetic counselling and genetic testing (in genetics services or in gynaecology oncology multidisciplinary services)
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page