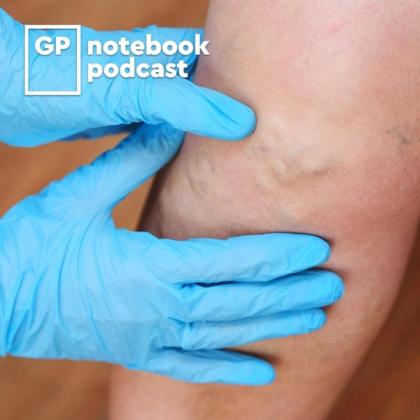
In this episode, Kevin considers the diagnosis and management of superficial venous thrombosis. Lesley is a 64-year-old woman who presents to us with a sore, itchy right leg and no past medical history of note. On examination, she has a tender, hard, erythematous varicose vein extending from her thigh to ankle. What should we do next? Should we be worried about underlying deep vein thrombosis?
Key references discussed in the episode:
- Nasr H, Scriven JM. BMJ. 2015;350:h2039. doi: 10.1136/bmj.h2039.
- NICE. Superficial vein thrombosis (superficial thrombophlebitis). 2020.
- Di Nisio M, Wichers IM, Middeldorp S. Cochrane Database Syst Rev. 2018;2(2):CD004982. doi: 10.1002/14651858.CD004982.pub6.
Key take-home messages from the episode:
- Superficial venous thrombosis (SVT) is the preferred term to superficial thrombophlebitis because the underlying pathology is that of thrombus formation rather than inflammation or infection.
- SVT shares risk factors with deep vein thrombosis (DVT) and pulmonary embolism (PE).
- If the SVT involves veins near the junction with the deep venous system, the risk of DVT and PE can reach nearly 20%.
- D-dimer is of no value in differentiating SVT from DVT.
- Consider referring all patients with clinical SVT of the lower limb for ultrasound scan.
- Individuals with below-knee SVT without evidence of DVT can be managed in primary care with non-steroidal anti-inflammatory drugs and compression.
- Individuals with SVT near the sapheno-femoral junction or sapheno-popliteal junction should be considered for surgical ligation or anticoagulation.
- Also consider anticoagulation if the superficial thrombus is >5 cm in length.
- Antibiotics have no role in the treatment of thrombophlebitis, except in clear cases of infection.
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page