In the Women's Health Initiative study there was a relative risk of 1.26 at 5.2 years of developing breast cancer (comparing oestrogen plus progestogen arm vs. placebo group) (1) - this meant an increased absolute risk of 8 per 10,000 women per year.
The Million Women Study (2) was set up to investigate the effects of specific types of HRT on incident and fatal breast cancer.Over one million UK women (1 084 110) aged 50-64 years were recruited into the Million Women Study between 1996 and 2001, provided information about their use of HRT and other personal details, and were followed up for cancer incidence and death. Results showed that:
- breast cancer was more likely in current users of HRT
- current users of HRT at recruitment were more likely than never users to develop breast cancer (adjusted relative risk 1.66 [95% CI 1.58-1.75], p<0.0001); also current users were more likely to die from breast cancer (1.22 [1.00-1.48], p=0.05). Note though that previous users of HRT were not at an increased risk of incident or fatal disease (1.01 [0.94-1.09] and 1.05 [0.82-1.34], respectively)
- breast cancer incidence was higher in users of oestrogen-progestagen preparations than other HRT preparations
- incidence of breast cancer was significantly higher for current users of preparations containing oestrogen only (1.30 [1.21-1.40], p<0.0001), oestrogen-progestagen (2.00 [1.88-2.12], p<0.0001), and tibolone (1.45 [1.25-1.68], p<0.0001), but the magnitude of the associated risk was much greater for oestrogen-progestagen than for other types of HRT (p<0.0001)
- increasing total duration of use for each type of HRT resulted in an increase in risk of a current HRT user developing breast cancer:
- 10 years' use of HRT is estimated to result in five (95% CI 3-7) additional breast cancers per 1000 users of oestrogen-only preparations
- 10 years' of HRT in the form of oestrogen-progestagen combinations is estimated to have resulted in 19 (15-23) additional cancers per 1000 users
A study of over 100,000 women diagnosed with breast cancer in relation to type and timing of menopausal hormone therapy and breast cancer risk was published in August 2019 (3). Based on this the MRHA has stated (4) :
in the UK about 1 in 16 women who never use HRT are diagnosed with breast cancer between the ages of 50 and 69 years. This is equal to 63 cases of breast cancer per 1000 women. Over the same period (ages 50-69 years), with 5 years of HRT use, the study estimated:
- about 5 extra cases of breast cancer per 1000 women using estrogen-only HRT
- about 14 extra cases of breast cancer per 1000 women using estrogen combined with progestogen for part of each month (sequential HRT)
- about 20 extra cases of breast cancer per 1000 women using estrogen combined with daily progestogen HRT (continuous HRT)
These risks are for 5 years of HRT use. The numbers of extra cases of breast cancer above would approximately double if HRT was used for 10 years instead of 5.
With respect to age of onset of use and HRT (4):
- risk of breast cancer depends on many factors, including age at menopause
- women who do not use HRT and who experience menopause between ages 40 and 50 years have a lower risk of breast cancer than women who experience menopause at a later age
- however, in women who start HRT in their 40s, the number of HRT-related breast cancers diagnosed by age 69 years is similar to that in women who use HRT for a similar duration starting in their 50s
- because women who have a menopause in their 40s have longer time as a current HRT-user plus ex-user before they are 69 years old
- not known if the increased risk of breast cancer with HRT use is similar for women who take HRT following a premature menopause (younger than age 40 years), or how their risk may be affected by any underlying conditions
- however, in women who start HRT in their 40s, the number of HRT-related breast cancers diagnosed by age 69 years is similar to that in women who use HRT for a similar duration starting in their 50s
MHRA has stated (4):
- All forms of systemic HRT are associated with a significant excess incidence of breast cancer, irrespective of the type of estrogen or progestogen or route of delivery (oral or transdermal)
- There is little or no increase in risk with current or previous use of HRT for less than 1 year; however, there is an increased risk with HRT use for longer than 1 year
- Risk of breast cancer increases further with longer duration of HRT use
- Risk of breast cancer is lower after stopping HRT than it is during current use, but remains increased in ex-HRT users for more than 10 years compared with women who have never used HRT
- Risk of breast cancer is higher for combined estrogen-progestogen HRT than estrogen-only HRT
- For women who use HRT for similar durations, the total number of HRT-related breast cancers by age 69 years is similar whether HRT is started in her 40s or in her 50s
- The study found no evidence of an effect on breast cancer risk with use of low doses of estrogen applied directly via the vagina to treat local symptoms
The MHRA has summarised the risks of HRT with respect to breast, endometrial and ovarian cancer (4):
Summary of HRT risks and benefits* during current use and current use plus post-treatment from age of menopause up to age 69 years, per 1000 women with 5 years or 10 years use of HRT (4)
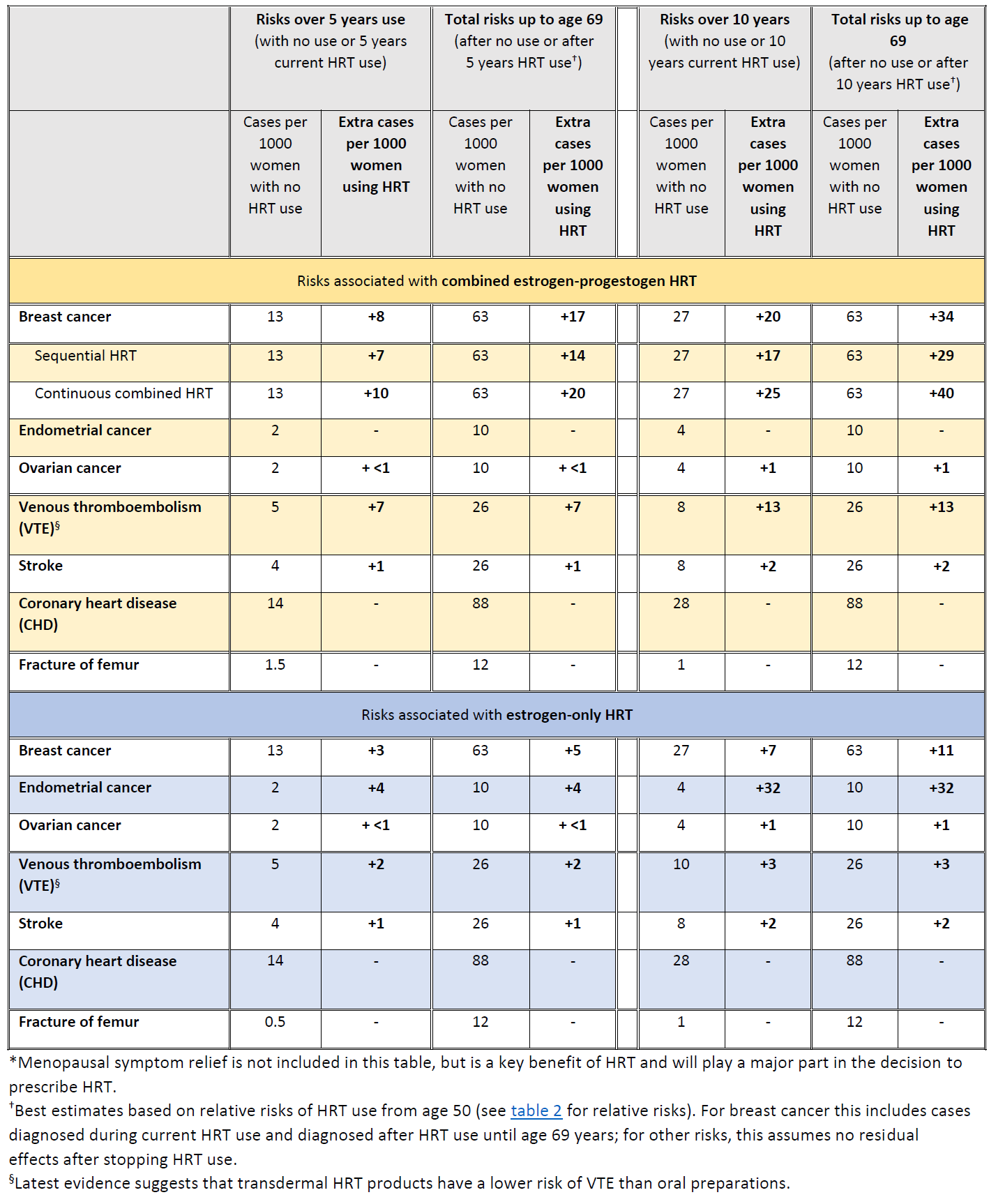
Review of the Evidence for Breast Cancer Risk and HRT (5,6,7,8,9):
The British Menopause Society (BMS), International Menopause Society (IMS), European Menopause and Andropause Society (EMAS), Royal College of Obstetricians and Gynaecologists (RCOG) and Australasian Menopause Society (AMS) have issued clarification of the evidence on the risk of breast cancer with menopausal hormone therapy (MHT) in response to the recommendations of the European Medicines Agency (EMA) - the central European drug regulatory body - Pharmacovigilance Risk Assessment Committee on 11-14 May 2020 that followed on from a meta-analysis by the Collaborative Group on Hormonal Factors in Breast Cancer (CGHFBC) published in the Lancet on 30 August 2019.
This advice is summarised below (5):
MHT and breast cancer risk – the CGHFBC meta-analysis Results from the CGHFBC meta-analysis show a small increase in the absolute risk of breast cancer: 5-years intake of MHT starting at the age of 50 years and risk of breast cancer at age 50-69 years
10-year intake of MHT starting at the age of 50 years and risk of breast cancer risk at age 50-69 years
|
Interpretation of the evidence on the risk of breast cancer with MHT
- the findings from the CGHFBC meta-analysis are in keeping with the NICE guidance 2015 analysis of the observational data on the risk of breast cancer and MHT
- the findings from the CGHFBC meta-analysis should be explained to women when discussing the benefits and risks of MHT. However, discussions on the risk of breast cancer with MHT should also include the findings from the WHI placebo-controlled randomized trials and the large E3N observational studies, which reported on the risk of breast cancer risk in users of micronized progesterone and dydrogesterone compared with other progestogens. Neither of the latter two studies was included in the CGHFBC meta-analysis
- the recently published WHI data showed a significant decrease in the risk of diagnosis of breast cancer with estrogen-only MHT and a significant reduction in breast cancer mortality compared with placebo
- women who took combined estrogen and progestogen MHT had an increased risk of breast cancer compared to placebo, in keeping with NICE guidance conclusions, but showed no significant difference in breast cancer mortality compared with placebo
- the E3N observational studies suggested a lower breast cancer risk in users of micronized progesterone and dydrogesterone compared to users of other progestogens
- the joint statement highlights that "
- " Recommendations on the risk of breast cancer with MHT should take into consideration the findings from the WHI randomized trials and the observational data on micronized progesterone and dydrogesterone from the E3N study as well as those from the CGHFBC meta-analysis
Informed consent:
- risk of breast cancer should be considered in the context of the overall benefits and risks associated with MHT intake including menopausal symptom control, improved quality of life and the long-term impact on bone and cardiovascular health. The decision whether to take MHT, the dose of MHT and the duration of its use should be made on an individualized basis after discussing the benefits and risks with women to help them make an informed choice about their health and care.
MHT and breast cancer risk - The CGHFBC meta-analysis (5)
Key points summary
• Only a small number of women on micronized progesterone were included. Therefore, conclusions regarding its impact on the risk of breast cancer diagnosis could not be determined from this meta-analysis.
|
There are a number of limitations in the methodology of the CGHFBC meta-analysis that need to be considered when interpreting the data. These include the following (5):
- 1. Some of the studies included in the CGHFBC meta-analysis had methodological limitations
- a key example of this is that one of the main studies contributing to the meta-analysis, the Million Women Study, had a significantly increased risk of breast cancer at 4 months from commencement of recruitment (RR 1.19; 95% CI 1.09 to 1.30 for users of estrogen-only and RR 1.41; 95% CI 1.31 to 1.52 for users of combined MHT). It is highly unlikely that breast cancer would develop within 4 months from recruitment and this would, therefore, suggest that a significant proportion of women had undetected breast cancer at the time of entry into the study; this should be considered when interpreting the findings from the CGHFBC meta-analysis
- a key example of this is that one of the main studies contributing to the meta-analysis, the Million Women Study, had a significantly increased risk of breast cancer at 4 months from commencement of recruitment (RR 1.19; 95% CI 1.09 to 1.30 for users of estrogen-only and RR 1.41; 95% CI 1.31 to 1.52 for users of combined MHT). It is highly unlikely that breast cancer would develop within 4 months from recruitment and this would, therefore, suggest that a significant proportion of women had undetected breast cancer at the time of entry into the study; this should be considered when interpreting the findings from the CGHFBC meta-analysis
- 2. The CGHFBC meta-analysis only included a very small number of women on micronized progesterone and it appears that the large observational data from the French E3N study which suggested that micronized progesterone is likely to be associated with a lower risk of invasive breast cancer compared to that noted with other progestogens were not considered in the meta-analysis
- 3. The CGHFBC meta-analysis did not report on breast cancer mortality
- long-term follow up of the WHI RCT up to 13 years showed no significant difference in breast cancer mortality or all-cause mortality with MHT compared with placebo
- WHO and Eurostat data showed a decline in European breast cancer mortality over the last three decades in women of all ages. This steady decline pre-dated by over a decade, the sustained worldwide fall in MHT prescribing following publication of WHI and the Million Women Study in the early 2000s. The reduction is likely to be related to treatment improvements and earlier diagnosis, including the impact of screening and is less likely to be related to the changing patterns in MHT use
- the WHI long-term randomized clinical trials, published in JAMA 2020, reported a significant reduction in breast cancer mortality with estrogen-only MHT and no significant difference in breast cancer mortality in women who took combined estrogen and progestogen MHT compared with placebo
"We believe that the findings from the CGHFBC meta-analysis should be explained to women when discussing the benefits and risks of MHT. However, discussions on the risk of breast cancer with MHT should also include the findings from the WHI placebo-controlled randomized trials and the large E3N observational studies, which reported on the risk of breast cancer risk in users of micronized progesterone and dydrogesterone compared with other progestogens. Neither of the latter two studies was included in the CGHFBC meta-analysis. (5)"
Vinogradova Y et al undertook a study of 98,611 women aged 50-79 with a primary diagnosis of breast cancer between 1998 and 2018, matched by age, general practice, and index date to 457,498 female controls (9):
- overall, 33,703 (34%) women with a diagnosis of breast cancer and 134,391 (31%) controls had used HRT prior to one year before the index date
- compared with never use, in recent users (<5 years) with long term use (>=5 years), oestrogen only therapy and combined oestrogen and progestogen therapy were both associated with increased risks of breast cancer (adjusted odds ratio 1.15 (95% confidence interval 1.09 to 1.21) and 1.79 (1.73 to 1.85), respectively)
- for combined progestogens, the increased risk was highest for norethisterone (1.88, 1.79 to 1.99) and lowest for dydrogesterone (1.24, 1.03 to 1.48)
- past long term use of oestrogen only therapy and past short term (<5 years) use of oestrogen-progestogen were not associated with increased risk
- risk associated with past long term oestrogen-progestogen use, however, remained increased (1.16, 1.11 to 1.21)
- in recent oestrogen only users, between three (in younger women) and eight (in older women) extra cases per 10,000 women years would be expected, and in oestrogen-progestogen users between nine and 36 extra cases per 10,000 women years
- for past oestrogen-progestogen users, the results would suggest between two and eight extra cases per 10,000 women years
A NIHR alert relating to the Vunogradova study states that (10):
- Most women took combined HRT, which was linked to a small increase in risk of breast cancer. The risk increased with:
- a woman’s age, with lower increases in risk for women in their 50s, compared to those in their 60s and 70s
- the duration of treatment, with lower increases in risk with HRT taken short-term (less than 5 years) than long-term (more than 5 years)
- current or more recent HRT treatment, which came with higher risks than past-use (more than 5 years ago)
- the type of progestogen in combined HRT; with the highest risks with norethisterone and the lowest with dydrogesterone.
- The researchers stressed that some women who had never taken HRT would still get breast cancer. For example, if a group of 10,000 women in their 50s had never taken HRT, 26 women would still get breast cancer in a year. If all 10,000 women had recently taken combined HRT for less than 5 years, 35 would get breast cancer. So, in this large group of women, the HRT is linked to 9 extra cases of breast cancer in a year. That is less than one in a thousand women.
- The increased risk was mostly linked to combined HRT, and the type of progestogen made a difference. Risk increased similarly when preparations containing some types of progestogen (norethisterone, levonorgestrel, or medroxyprogesterone) were taken for more than a year. The lowest increase in risk was with dydrogesterone (another type of progestogen).
- Even if women took combined HRT long-term (more than 5 years), risks reduced after therapy was stopped. For women in their 50s, there was no extra risk of breast cancer with combined HRT that was stopped more than 5 years previously. There was little extra risk among women in their 60s and 70s.
- There was no increased risk of breast cancer:
- with any current HRT taken for one year or less
- with past use of oestrogen-only HRT, even if taken long-term
- with past use of combined HRT taken short-term.
Reference:
- Writing Group for the Women's Health Initiative Investigators. Risks and benefits of estrogen plus progestin in healthy postmenopausal women. Principal results for the Women's Health Initiative Randomized controlled trial. JAMA 2002; 288:321-33
- Lancet 2003; 362: 419-27
- Collaborative Group on Hormonal Factors in Breast Cancer. Type and timing of menopausal hormone therapy and breast cancer risk: individual participant meta-analysis of the worldwide epidemiological evidence. The Lancet. Published August 29, 2019.
- MHRA (August 2019). Hormone replacement therapy and risk of breast cancer
- BMS, IMS, EMAS, RCOG and AMS Joint Statement on menopausal hormone therapy (MHT) and breast cancer risk in response to EMA Pharmacovigilance Risk Assessment Committee recommendations in May 2020
- Collaborative Group on Hormonal Factors in Breast Cancer. Type and timing of menopausal hormone therapy and breast cancer risk: individual participant meta-analysis of the worldwide epidemiological evidence. Lancet 2019;394:1159-68. doi: 10.1016/S0140-6736(19)31709-X 31474332.
- Chlebowski RT, Anderson GL, Aragaki AK, et al. Association of Menopausal Hormone Therapy With Breast Cancer Incidence and Mortality During Long-term Follow-up of the Women’s Health Initiative Randomized Clinical Trials. JAMA. 2020;324(4):369–80. doi: 10.1001/jama.2020.9482
- Fournier A, Mesrine S, Dossus L, et al. Risk of breast cancer after stopping menopausal hormone therapy in the E3N cohort. Breast Cancer Research and Treatment 2014;145(2):535–43
- Vinogradova Y, Coupland C, Hippisley-Cox J. Use of hormone replacement therapy and risk of breast cancer: nested case-control studies using the QResearch and CPRD databases. BMJ 2020;371:m3873.
- https://evidence.nihr.ac.uk/alert/risk-of-breast-cancer-with-hrt-depends-therapy-type-and-duration/
Related pages
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page