Seminomas have a good prognosis:
- they are radiosensitive
- there is a >90% cure rate for stage I and stage II disease
- it remains localised for long periods before spreading to lymph nodes
- haematogenous spread occurs late
Teratomas offer a worse prognosis:
- with no trophoblastic element, there is a 90% cure rate for stage I disease
- but 60% present with stage II - IV disease
- haematogenous spread occurs early
- yolk sac or choriocarcinomic elements are poor prognostic indicators
For all tumours, even when it has metastasised, has a crude overall five-year survival rate in Scotland of 95.8% (1)
UK statistics:
- almost all (98%) men diagnosed with testicular cancer in England and Wales survive their disease for ten years or more (2010-11)
- almost all (98%) men diagnosed with testicular cancer in England and Wales survive their disease for five years or more (2010-11)
- around all (99%) men diagnosed with testicular cancer in England and Wales survive their disease for one year or more (2010-11)
- almost all men in England diagnosed with testicular cancer aged 15-49 survive their disease for five years or more, compared with more than two-thirds of men diagnosed aged 80 and over (2009-2013)
- testicular cancer survival is improving and has increased in the last 40 years in the UK, probably because of combination chemotherapy
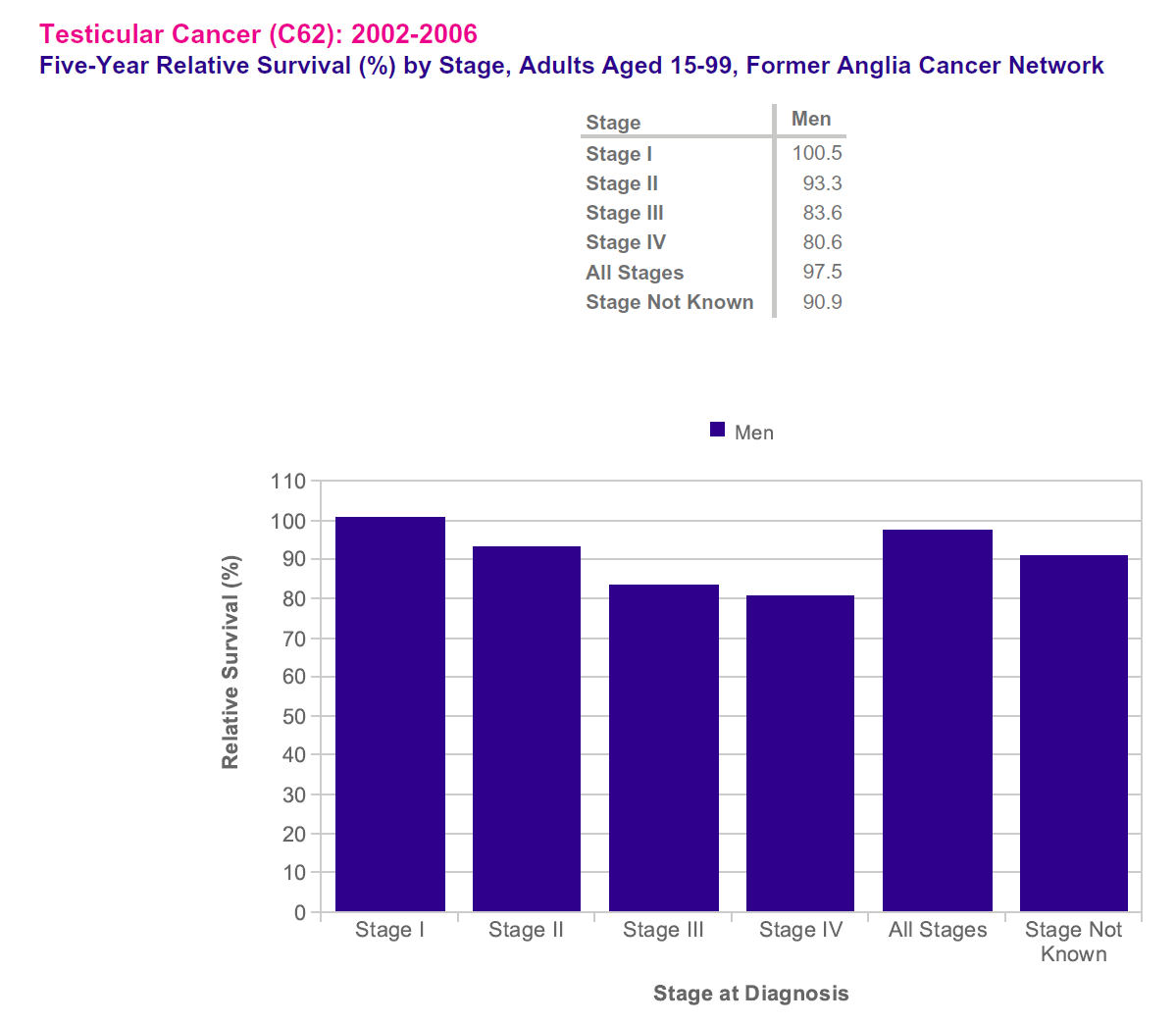
- in the 1970s, around 7 in 10 men diagnosed with testicular cancer survived their disease beyond ten years, now it's around all men. When diagnosed at its earliest stage, all men with testicular cancer will survive their disease for five years or more, compared with around 8 in 10 men when diagnosed at the latest stage
Risk of recurrence of testicular cancer after treatment for testicular cancer:
- hypothesized that cisplatin-based chemotherapy (CBCT) reduces the occurrence of metachronous contralateral (second) germ cell testicular cancer (TC)
- a study (3) showed overall, the 20-year crude cumulative incidence was 4.0% (95% CI, 3.5 to 4.6), with lower incidence after chemotherapy (CT) (3.2%; 95% CI, 2.5 to 4.0) than after surgery only (5.4%; 95% CI, 4.2 to 6.8)
- second TC incidence was also lower for those age >= 30 years (2.8%; 95% CI, 2.3 to 3.4) at first TC diagnosis than those age < 30 years (6.0%; 95% CI, 5.0 to 7.1)
- overall, the second TC risk was 13-fold higher compared with the risk of developing TC in the general male population (standardized incidence ratio, 13.1; 95% CI, 11.5 to 15.0)
Reference:
- 1) SIGN (March 2011). Management of adult testicular germ cell tumours.
- 2) CRUK. Testicular Cancer Statistics
- 3)Hellesnes R et al. Metachronous Contralateral Testicular Cancer in the Cisplatin Era: A Population-Based Cohort Study. DOI: 10.1200/JCO.20.02713 Journal of Clinical Oncology 2020.
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page