DABIGATRAN
Consult SPC for detailed guidance before prescribing.
Dabigatran is a direct thrombin inhibitor and is available as 75mg, 110mg and 150mg capsules.
Indications (1,2)
- Stroke prevention in non-valvular atrial fibrillation
- Prevention of thromboembolism total knee replacement (TKR) and total hip replacement (THR)
- Treatment of DVT and PE
- Prevention of recurrent DVT and PE
Contra-indications (1,2)
Active bleeding; significant risk of major bleeding (e.g. recent gastro-intestinal ulcer, oesophageal varices, recent brain, spine, or ophthalmic surgery, recent intracranial haemorrhage, malignant neoplasms, vascular aneurysm, haemorrhagic stroke); do not use as anticoagulant for prosthetic heart valve
Initiation
- Baseline Activated Partial Prothrombin Time (aPTT), International Normalised Ratio (INR), haemoglobin, urea & electrolytes and liver function tests
- Weigh patient and obtain height
- Calculate baseline creatinine clearance (CrCl) using Cockgroft and Gault
- If changing from another anticoagulant to dabigatran then follow the guidance below:
- Parenteral anticoagulants to dabigatran Dabigatran should be given 0-2 hours prior to the time that the next dose of the alternate therapy would be due, or at the time of discontinuation in case of continuous treatment (e.g. intravenous Unfractionated Heparin (UFH))
- VKA to dabigatran Stop the VKA. Give dabigatran as soon as the INR is <2.0.
Dagibatran dosing guidance (3):
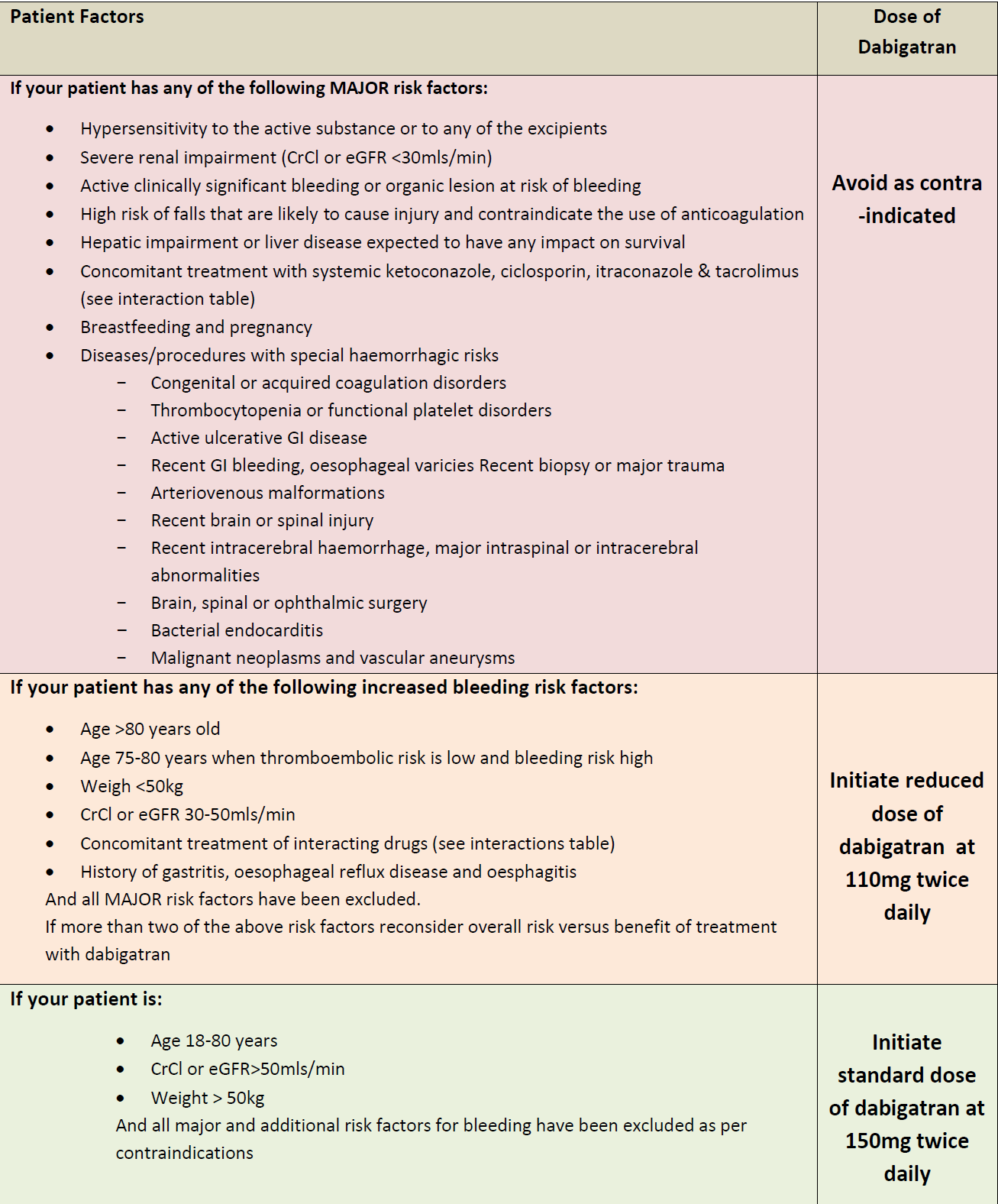
Monitoring (1)
No monitoring is required to ensure therapeutic levels but regular monitoring of CrCl recommended to avoid accumulation of dabigatran in reduced renal function. Dabigatran must be discontinued where CrCl<30ml/min.
For patients at risk of bleeding the aPTT provides an approximate indication of the anticoagulant intensity achieved with dabigatran. This test has limited sensitivity and is not suitable for precise quantification of anticoagulant effect, especially at high plasma concentrations of dabigatran. High aPTT values should be interpreted with caution. There is no requirement to monitor aPTT.
Adverse effects
Dabigatran should be used with caution in conditions with an increased risk of bleeding. Bleeding may occur at any site during therapy with dabigatran. An unexplained fall in haemoglobin and/or haematocrit or blood pressure should lead to an investigation to identify a bleeding site. Close clinical surveillance is recommended throughout the treatment period, especially if risk factors are combined
Nausea, dyspepsia, diarrhoea, abdominal pain, anaemia, haemorrhage less commonly hepatobiliary disorders, vomiting, dysphagia, gastro-intestinal ulcer, gastro-oesophageal reflux, oesophagitis, thrombocytopenia
Discontinuation of therapy
If patient has reached end of duration of treatment then dabigatran can be discontinued immediately. Where switching from dabigatran to alternative anticoagulant follow the guidance in the SPC. If stopping dabigatran for inpatients then ensure VTE assessment is redone.
If changing from dabigatran to another anticoagulant then follow the guidance below:
- Dabigatran treatment to Vitamin K antagonists (VKA) e.g. warfarin. Adjust the starting time of the VKA based on CrCl as follows:
- CrCl >=50 ml/min, start VKA three days before discontinuing dabigatran
- CrCl 30 - < 50 ml/min, start VKA two days before discontinuing dabigatran
- Dabigatran treatment to parenteral anticoagulant. It is recommended to wait 12 hours after the last dose before switching from dabigatran to a parenteral anticoagulant. If CrCl < 30mls/min wait 24 hours before initiating parenteral treatment
Reference:
- Wirral University Teaching Hospital NHS Trust. Oral Anticoagulants (VKA and DOAC) Guidelines for prescribing, monitoring and management (Accessed 23/4/19)
- NHS Specialist Pharmacy Service (October 2017). Suggestions for Drug Monitoring in Adults in Primary Care
- West Cheshire Commissioning Group (April 24th 2019). Prescribing Guidance for Dagibatran.
Related pages
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page