Red legs are frequently seen in primary care but are often misdiagnosed. With a need for antimicrobial stewardship, it is important to identify the cause, rather than automatically rely on antibiotic prescription. Importantly, all that is red is not cellulitis; venous or varicose eczema is a common cause of swollen and red legs and requires a different management approach. In this episode, Dr James Waldron is joined by Dr Mark Graham (GP from Nottingham with experience in dermatology) to explore how to invest time initially to achieve the right diagnosis. The discussion considers differential diagnoses, clinical examination and management.
Key take-home points
- Red legs are a common presentation and whilst they can be cellulitis and treated with antibiotics, this is often not the case.
- Other possible differential diagnoses include venous eczema (also known as varicose or stasis eczema), deep-vein thrombosis or arterial insufficiency.
- Key differentiating features for cellulitis are that the skin feels hot, and it typically affects only one leg.
- For patients being seen in the community by nurses or carers, it is often worth a physical review by a GP to consider diagnosis, as doing so remotely can be challenging.
- Venous eczema is a fairly common problem in older patients, caused by impaired venous circulation driving a hypoxic environment, with waste products and oedema impacting the skin, ultimately causing inflammation and redness.
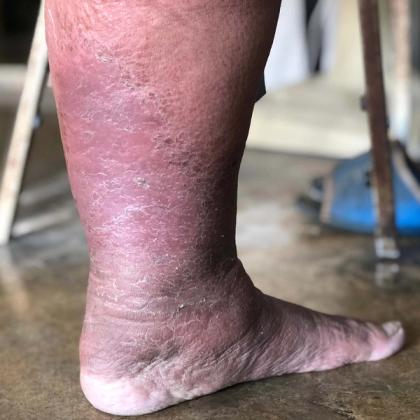
- The legs will both look the same, with redness to the skin but normal temperature to the touch and likely with oedema and varicose veins; there may also be scale.
- A test is to lie the patient down and elevate the leg to 90 degrees; after a few minutes, the redness may fade, confirming that there is venous congestion.
- Patients with decreased mobility are more at risk for venous eczema, and it is also more common in heart failure and after some joint replacement surgeries.
- Furosemide is often used in people with swollen legs to treat oedema, but it can affect renal function and blood pressure.
- Another consideration is that swollen legs are a side effect of amlodipine, which is commonly used to treat hypertension; switching to another agent or stopping all together may be appropriate.
- Untreated venous eczema can progress to leg ulcers; these should not be routinely swabbed.
- Compression is an important part of management for venous ulcers and also in venous eczema, helping to improve the venous return.
- A short course of furosemide 20–40 mg for a few weeks can be useful to help reduce the swelling before beginning compression, alongside topical steroids such as betamethasone valerate 0.1% twice daily, or mometasone.
- Ankle brachial pressure index can be used to check if it is safe to escalate to class II compression.
- Venous eczema can co-exist with cellulitis, in which case both need managing.
Helpful resources
- Wounds. https://wounds-uk.com/.
- NICE. 2020. https://www.nice.org.uk/guidance/ng152.
- Yosipovitch G, et al. Am J Clin Dermatol. 2023;24(2):275-286. doi:10.1007/s40257-022-00753-5.
- Cranendonk DR, et al. Neth J Med. 2017;75(9):366-378.
- Sullivan T, de Barra E. Clin Med (Lond). 2018;18(2):160-163. doi:10.7861/clinmedicine.18-2-160.
- British National Formulary. https://bnf.nice.org.uk/drugs/furosemide/.
Disclaimer
This content is for medical education purposes only and does not constitute clinical advice. While specific drugs and dosages may be discussed, clinicians should always refer to local protocols and official prescribing information before administering medication.
Create an account to add page annotations
Add information to this page that would be handy to have on hand during a consultation, such as a web address or phone number. This information will always be displayed when you visit this page